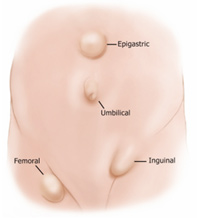
 A hernia can occur if there is a weakness in a part of the muscle layer that encloses and supports the abdominal organs, such as the bowel and stomach. A hernia can be identified as a lump that is felt under the skin at the site of the weakness in the muscle layer. Quite commonly the lump will appear when movement or straining causes the abdominal contents to be pushed through the area of weakness.
A hernia can occur if there is a weakness in a part of the muscle layer that encloses and supports the abdominal organs, such as the bowel and stomach. A hernia can be identified as a lump that is felt under the skin at the site of the weakness in the muscle layer. Quite commonly the lump will appear when movement or straining causes the abdominal contents to be pushed through the area of weakness.
The most common site of a hernia is in the groin. The hernia will protrude through a natural small weakness in the abdominal wall, where in men the blood vessels supplying the testes travel from inside the body through the abdominal wall in the groin, and into the scrotum.
Other common sites for a hernia include around the umbilical region where there is a natural weakness of the tissues. These hernias are more common in women after pregnancy or in people who are overweight.
An incisional hernia can occur through the previous abdominal scar, again through a natural area of weakness of the abdominal wall.
A hiatus hernia is a weakness in the diaphragm which leads to a protrusion or herniation of the stomach from the abdomen through into the thorax. These hernias are commonly associated with heartburn type symptoms.
When you see Mr Jenkinson in the outpatients’ clinic you may well forget some of the answers that he gave to your questions. We have therefore taken the commonly asked questions by patients from each of the procedures and added Mr Jenkinson’s answers.
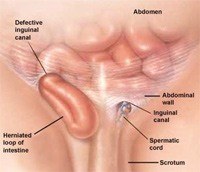
A groin hernia is caused by a weakness in the muscle layer of the abdominal wall in the groin. This causes a protrusion of tissue through the weakness, resulting in the feeling of a lump in the groin. The hernia can sometimes just be associated with pain.
A hernia is more likely to occur with increased intra-abdominal pressure. This can be due to weight lifting in the gym or a job that involves heavy lifting, anyone who has a chronic cough or chronic constipation, pregnancy and obesity. Hernias can also run in families. Commonly, however, there is no apparent cause for the development of a hernia.

Most hernias will increase in size over time. The visible increase in size can be over a matter of weeks, months or years. As the size increases the hernia will tend to become more painful.
There is a small chance that intra-abdominal tissue (bowel or fatty tissue) can get stuck inside the hernia. If the blood supply to this tissue is then compromised, strangulation of the tissue can occur and the hernia will become very painful. In these cases, urgent medical attention is necessary and open operation would be required to repair the hernia and check on whether the trapped tissue is viable or needs to be removed. This situation is called a strangulated hernia.
Groin hernias can be repaired via either the traditional open operation or a laparoscopic keyhole approach.
The laparoscopic method of repairing a hernia requires much less cutting of the tissues. Therefore there is significantly less pain after the operation compared to an open groin hernia repair, and also a person will be much more likely to return to normal activities faster.
References: Prospective randomised controlled trial of laparoscopic versus open inguinal hernia repair: five year follow up. Wellwood JM et al. BMJ 2003. May 10; vol 326 (7397), 1012-3
Outcomes in patients who underwent both laparoscopic and open inguinal hernia repairs. Bernardotto M, Jenkinson A. ANZ J Surg. 2010 May;80(5):381-2.
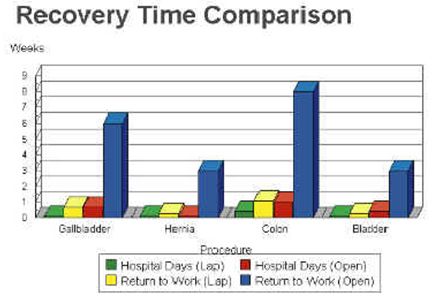
This chart compares the difference in recovery time and return to work between laparoscopic and open surgery.
In addition to this, the traditional open hernia repair has been shown to have a fairly high risk of causing chronic groin numbness or chronic groin pain in the long term following surgery. This is because in open surgery the supporting mesh is placed in the proximity of the nerves of the groin, and therefore it is not uncommon for these nerves to be trapped as scar tissue develops around the mesh. In the laparoscopic approach the mesh is placed in a deeper layer of the muscle wall, which is away from these nerves.
The risks of complications following a laparoscopic hernia repair are very low. The most common risks are of bleeding or bruising around the three small abdominal wounds, or a discharge through the umbilical wound for a few days. The risk of recurrence of a hernia following laparoscopic or open hernia repair has been shown to be the same in the hands of experienced surgeons. In both the open and laparoscopic repair there is a very small chance of damage to organs or damage to the blood supply to the testicle. The risk of these complications is negligible in the hands of a very experienced surgeon.
Laparoscopic hernia repair is performed under general anaesthetic. The procedure takes approximately 30 minutes. There are three small cuts in the abdomen. A 10 mm cut within the umbilicus and two 5 mm cuts either side of the umbilicus at the same level.
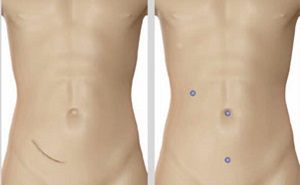
Comparison of the scars in open and laparoscopic hernia repair
The hernia is visualised with a telescopic camera. It is reduced with specialised laparoscopic instruments and a mesh is placed over the weakness in the abdominal wall.
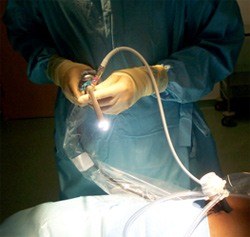
Photograph of the 10mm diameter telescope with light source and digital camera
A patient can go home either on the same day of surgery or after an overnight stay.
Pain is much less following laparoscopic hernia repair compared to an open hernia repair. There will be a bruising sensation in the groin. This pain should be well controlled with the painkillers that you were prescribed on discharge from hospital. You may need to take painkillers for one or two weeks following the operation but should be able to return to work and light activities within a few days of surgery.
Following laparoscopic hernia surgery a person should be able to increase their activity levels within days of the operation. This would include longer and longer walks and more activity around the house. Introduction of aerobic activity in the gym would be encouraged one week after surgery. Lifting of heavy weights needs to be avoided for one month after surgery.
A sports hernia has been described as a tear in the muscle and ligaments of the groin (conjoint tendon). This leads to quite severe pain on running, kicking and crouching activities. It therefore differs from a traditional inguinal hernia, which is due to an actual weakness in the groin, and causes a lump. A sports hernia or Gilmore’s groin, as it is sometimes described, is a musculoligamentous tear and not an out and out weakness of the muscle wall.
The diagnosis of a sports hernia can be very subjective amongst doctors and the diagnosis and treatment options can vary if different opinions are sought. It is for this reason that careful diagnosis and exclusion of other conditions in the groin should be performed before any treatment is discussed.
It can be quite difficult to diagnose a sports hernia via even high resolution CT imaging or MRI imaging. Therefore often the diagnosis is by exclusion of other conditions that can cause similar symptoms. These conditions include a strain or partial avulsion of the adductor longus muscle in the groin or osteitis pubis, which is a chronic inflammatory condition of the hip girdle caused by excessive exercise and strain in this area.
Both of these conditions can be diagnosed by CT or MRI, and it is for this reason that these investigations should be performed before a diagnosis of exclusion of sports hernia is made.
Sports doctors and surgeons have different opinions on the best treatment option for a sports hernia. Gilmore’s operation, which was similar to an open old fashioned hernia repair, involved a direct suture of the tear in the groin muscle if it was identified. It also involved a suturing and strengthening of the back wall of the muscle layer and probably a disruption of some of the nerves traversing the groin, which helped to improve the pain associated with the condition.
Some surgeons may advocate a laparoscopic hernia repair if the initial investigations show there is evidence of a weakness in the abdominal wall, associated with the typical groin pain of sports hernia. A therapy to just tackle the pain of the area could include injection of local anaesthetic and steroid into the nerves of the groin. If this is successful at alleviating symptoms then radiofrequency ablation of these nerves can be contemplated.
Despite all these treatment options, many sports doctors, physiotherapists and surgeons still advocate rest and physiotherapy as the best treatment for sports hernia or Gilmore’s groin. It is interesting that open hernia repair advocates an extended period of rest following the procedure, and this may well be one of the reasons that some athletes seem to be better following their convalescence from surgery.
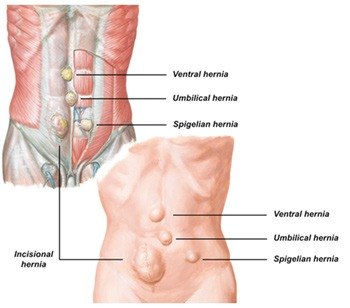
Hernias that occur in the abdominal wall are not unusual. The most common of these hernias is the umbilical hernia. In the midline above the umbilicus a ventral or epigastric hernia can occur. Hernias through a previous abdominal wall scar occur in 20% of cases.
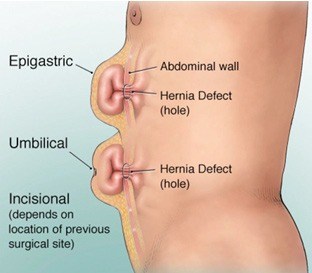 An umbilical hernia is a weakness in the muscles and ligaments around the umbilical area. These hernias can be present at birth or more commonly will develop during adult life. Any condition that increases the pressure within the abdomen can contribute to the development of an umbilical hernia. Therefore these hernias are more common after pregnancy, in people who have central abdominal obesity, in weight lifters or those whose job involves heavy lifting and people with a chronic cough or constipation. In addition to this there may be a natural family predisposition to a hernia in this area.
An umbilical hernia is a weakness in the muscles and ligaments around the umbilical area. These hernias can be present at birth or more commonly will develop during adult life. Any condition that increases the pressure within the abdomen can contribute to the development of an umbilical hernia. Therefore these hernias are more common after pregnancy, in people who have central abdominal obesity, in weight lifters or those whose job involves heavy lifting and people with a chronic cough or constipation. In addition to this there may be a natural family predisposition to a hernia in this area.
If a hernia is small and measures 1 cm diameter or less and the hernia is not causing symptoms then they do not need to be repaired. However invariably these hernias will get bigger in time and may then become painful. The decision on whether to operate or not should be taken after discussion in the outpatients’ clinic on the advantages and risks of surgery versus those of not operating.
If an umbilical hernia measures less than 2 cm diameter at its base then I would repair them using a very simple and safe open technique, whereby a small cut is made in the upper crease of the umbilicus. The hernia is pushed back inside the abdomen and the weakness is repaired with simple suturing. If the hernia is larger than 2cm then I would recommend a laparoscopic, or key hole surgery technique to repair it. This involves 3 small cuts measuring 5 to 10mm in the left side of the abdomen. The hernia is reinforced with a lightweight mesh which is secured on the inside underneath the hernia. The mesh encourages scar tissue to form and therefore strengthens the whole area, decreasing the chance of a recurrence of the hernia.
Most patients will be discharged from the hospital either on the same day of surgery or the morning after surgery with one overnight stay.
There is some initial bruising sensation which is well controlled with simple painkillers. This discomfort improves within days of surgery.
This procedure has a very low risk. There may be a small chance of bruising or a low grade infection in the wound following an open operation. With a laparoscopic procedure there are very low risks of bleeding, damage to the bowel or adhesion formation. The risk of recurrence of the hernia after operation is low but the chance of recurrence would be increased in patients who have increased intra-abdominal pressures, such as those with central obesity or after further pregnancy.
Most people will be back out to work within days or one week of surgery.
Aerobic exercise such as running, cycling and swimming can be resumed within days of surgery.I would advise that patients refrain from heavy lifting of weights or suitcase etc. for six weeks after surgery to decrease the chance of the hernia recurring.
Incisional hernias can occur after any type of abdominal operation.The hernia or weakness in the abdominal wall covering occurs through an area where the previous operation has occurred, and the surgeon has sutured the muscle layers together.Incisional hernias can occur in up to 20% of patients who have had previous operations in the abdomen.
If the hernia occurs within a few days of an operation, then it may well be that the stitches that the surgeon placed have pulled through the tissue and become loose.Alternatively, if an infection develops after an operation it is more likely that an incisional hernia will occur quite soon after surgery.In the longer term a hernia may develop at the site of a previous operation in a patient who has increased intra-abdominal pressure.This would include patients who are centrally obese, have had many pregnancies, are involved in lifting heavy weights, either through the gym or at work, and those that have a chronic cough or chronic constipation.
The decision on whether to repair an incisional hernia is based on how big the hernia is, whether it is causing any symptoms such as pain, and whether there is any long term risk of bowel strangulation within the hernia.If a hernia is small and asymptomatic with no long term risk, then a decision can be made to watch and wait to see if it becomes larger or more symptomatic.Clearly if a hernia is causing pain or there is a risk of strangulation of bowel, then it requires surgical repair.
An incisional can be repaired via a simple open operation, a laparoscopic operation or a combined laparoscopic and open operation.
If the hernia is small then hospital stay will probably be only one night.For larger hernia repairs hospital stay may be several nights.
There will be some pain and discomfort in the area of the operation but this should be well controlled with painkillers.This bruising sensation will decrease within a few days to a week of surgery.Depending on the size of the hernia, painkillers would need to be taken for one or two weeks.
This procedure has a very low risk.There may be a small chance of bruising or a low grade infection in the wound following an open operation. With a laparoscopic procedure there are very low risks of bleeding, damage to the bowel or adhesion formation.The risk of recurrence of the hernia after operation is low but the chance of recurrence would be increased in patients who have increased intra-abdominal pressures, such as those with central obesity or after further pregnancy.
For small incisional hernias you can resume work within a few days of surgery.However large hernias requiring more complex surgery you may need to take two weeks off work.
I would encourage exercise within days of surgery, increasing activity around the house and walking distance.Aerobic exercise in the form of jogging, cycling or swimming can be started within a week of surgery.Any heavy lifting of weights or suitcases should be avoided for six weeks after surgery until the scar tissue in the hernia repair has become strong enough to prevent the hernia recurring.