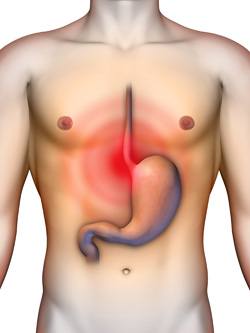
 Everyone has experienced the uncomfortable feeling of heartburn when acid refluxes from the stomach into the oesophagus (gullet). To experience this occasionally is normal and is associated with belching to release gas from the stomach.
Everyone has experienced the uncomfortable feeling of heartburn when acid refluxes from the stomach into the oesophagus (gullet). To experience this occasionally is normal and is associated with belching to release gas from the stomach.
However, if acid regurgitation into the oesophagus becomes more frequent, it can start to have a detrimental effect on a person’s health and sense of wellbeing. This condition is termed acid reflex disease, or in medical language, gastro-oesophageal reflux disease.
There are many misconceptions regarding heartburn and acid reflux that I would like to address. The following section will attempt to answer common questions that patients will ask in clinic, and explain more fully exactly how acid reflux is caused, the relationship between acid reflux and hiatus hernia, what Barrett’s oesophagus is and the best treatment options for acid reflux.
The good news about acid reflux disease is that if it is investigated appropriately and diagnosed accurately, then there are extremely good treatment options both through drug therapy or safe surgery. Therefore if reflux symptoms are currently a problem, you can be reassured that soon you will be able to return to a normal lifestyle.
When you see Mr Jenkinson in the outpatients' clinic you may well forget some of the answers that he gave to your questions. We have therefore taken the commonly asked questions by patients from each of the procedures and added Mr Jenkinson's answers.
Acid reflux disease is caused when stomach contents (acid and bile) reflux upwards past a weakened sphincter (valve mechanism) into the lower gullet.
Occasional acid reflux is a normal occurrence however when it occurs too frequently it can cause disabling symptoms and damage to the gullet.
The parts of the mechanism for swallowing and avoiding reflux can be thought of a muscular pump (the oesophagus), valve (the lower oesophageal sphincter or LOS) and reservoir (the stomach). If any of these three parts are defective then acid reflux can become more common.
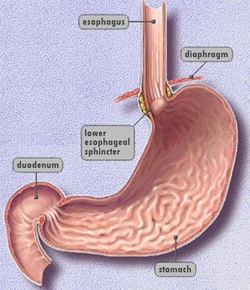
The reflux mechanism can be caused by an abnormality in either the oesophageal pump, the sphincter between the oesophagus and stomach, or the speed of emptying of the stomach reservoir.
The most common abnormality is a weakness in the valve (LOS). This accounts for about 80% of patients with reflux disease. Less commonly, there can be an abnormality in the effectiveness of the oesophageal pump or delayed emptying of the stomach.
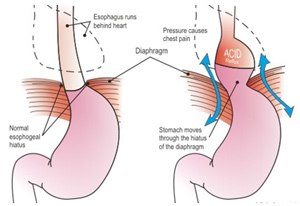 In normal anatomy the oesophagus passes from the chest cavity into the abdominal cavity through a small hole in the diaphragm. A hiatus hernia occurs when this hole becomes bigger and the ligaments attaching the diaphragm to the oesophagus becomes lax. Because the abdominal pressure is greater than the chest cavity pressure, the oesophagus and upper stomach push through the diaphragm from the abdomen into the chest.
In normal anatomy the oesophagus passes from the chest cavity into the abdominal cavity through a small hole in the diaphragm. A hiatus hernia occurs when this hole becomes bigger and the ligaments attaching the diaphragm to the oesophagus becomes lax. Because the abdominal pressure is greater than the chest cavity pressure, the oesophagus and upper stomach push through the diaphragm from the abdomen into the chest.
Hiatus hernias are common in everyday life. They will affect approximately 20% of people. As a person gets older it is more likely that they will develop a hiatus hernia. A hiatus hernia can cause a weakness of the valve between the oesophagus and stomach that normally prevents acid reflux. Therefore if a person has severe acid reflux caused by a hiatus hernia, then it is likely that a surgical operation to fix this anatomical abnormality will help resolve a person’s symptoms.
The three most common symptoms associated with reflux of acid into the oesophagus are:
These are the three most common symptoms that doctors will associate with reflux disease, however there are several much less common symptoms that can be caused by acid reflux that may be missed by your doctor. These include:
The presence of symptoms suggesting that you have acid reflux does not always mean that you definitely have this condition. There are a number of other conditions which have similar symptoms and therefore in order to plan proper treatment, you will require some tests or investigations to confirm the diagnosis.
 The most common test for reflux disease is the gastroscopy (oesophago-gastro-duodenoscopy or OGD). This involves looking at the oesophagus and stomach through a flexible endoscope. This procedure is a day case and is usually performed with anaesthetic throat spray but occasionally with sedation. The procedure takes only a matter of minutes to perform but will accurately show whether there is any damage to the oesophagus in the form of oesophagus or Barrett’s oesophagus. The gastroscopy will also show the presence or absence of a hiatus hernia that may be contributing to the acid reflux.
The most common test for reflux disease is the gastroscopy (oesophago-gastro-duodenoscopy or OGD). This involves looking at the oesophagus and stomach through a flexible endoscope. This procedure is a day case and is usually performed with anaesthetic throat spray but occasionally with sedation. The procedure takes only a matter of minutes to perform but will accurately show whether there is any damage to the oesophagus in the form of oesophagus or Barrett’s oesophagus. The gastroscopy will also show the presence or absence of a hiatus hernia that may be contributing to the acid reflux.
If the gastroscopy does not show any abnormality in the oesophagus caused by acid reflux, then further investigation with measurement of the pressures in your oesophagus and direct measurement of acid reflux over 24 hours using a sensor can be recommended.
This test is called oesophagus manometry and 24 hour pH measurement. It involves the placement of a thin plastic pressure tube through the nose and into the oesophagus and stomach. The technician performing the test will measure the effectiveness of the oesophageal pump mechanism whilst you swallow sips of water. The pressure in the lower oesophagus sphincter or valve between the oesophagus and stomach is also measured. The presence or absence of a hiatus hernia can be identified from this test.
After this part of the test, which normally takes half an hour, the pressure tube is removed and a thinner acid sensing tube is placed again through the nose into the stomach via the oesophagus. This tube is connected to a recording box that is worn on the belt. The patient is asked to continue normal activities for 24 hours with the sensor tube in place and press a button on the recording box when symptoms occur. The test will show in detail the exact amount of acid over a 24 hour period that has refluxed from the stomach into the oesophagus. It will also show whether or not there is a strong correlation between the symptoms that you experience and acid reflux events.
This test is considered the gold standard investigation by doctors for the diagnosis of acid reflux disease. It will also have the advantage of showing any abnormality in the oesophagus pump mechanism which may make your surgeon consider surgical options more carefully.
The third investigation that sometimes is considered for acid reflux disease is the barium swallow and meal. This involved the swallowing of a liquid which shows up on an X-ray video camera. The test would involve looking at the images to see whether the X-ray liquid refluxes back into the oesophagus, particularly when the patient is tipped slightly head down. Although this used to be quite a common investigation for reflux disease, it has now been superseded by a manometry and pH measurement and is much less commonly used. However if your doctor thinks you might have a big hiatus hernia, he may want to check on the exact anatomy of the area, and this can be performed much more accurately through this X-ray investigation.
 Occasionally if your doctor thinks that the cause of the acid reflux is not the oesophagus pump or the oesophagus sphincter (valve mechanism) but is due to an abnormality of stomach emptying, he may organise a test for this. These tests are called gastric emptying studies and involve the consumption of a meal followed by breath testing at regular intervals after this.
Occasionally if your doctor thinks that the cause of the acid reflux is not the oesophagus pump or the oesophagus sphincter (valve mechanism) but is due to an abnormality of stomach emptying, he may organise a test for this. These tests are called gastric emptying studies and involve the consumption of a meal followed by breath testing at regular intervals after this.
Before any of these tests are considered, it may well be that you will be asked to take a trial of a strong acid suppression drug to ascertain whether this improves your symptoms. If acid suppression cures your symptoms then it can be concluded that you do indeed have acid reflux disease. This may in itself be used as a diagnostic test and I would consider this to be the easiest and least uncomfortable option and one that maybe should be considered first.
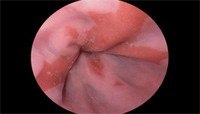
The continuous contact of acid onto the oesophagus can eventually cause damage to its lining. Most commonly this is in the form of soreness and inflammation (oesophagitis). This can span from a mild inflammation to a severe inflammation causing ulceration and bleeding of the lining of the oesophagus. Further complication of severe oesophagus can be the development of a stricture or narrowing in the lower oesophagus causing increasing difficulty with swallowing. A further complication is the development of a condition called Barrett’s oesophagus.
As well as local effects on the oesophagus itself, chronic acid reflux can cause asthma, recurrent chest infections, hoarseness, laryngitis and chronic coughing.
Conservative Treatment or Lifestyle Changes
Treatment of acid reflux and its symptoms should start with some changes in lifestyle that may be all that is required. These changes would include avoiding foods and drinks that may contribute to acid reflux episodes such as; caffeine, alcohol, spicy foods and chocolate and stopping smoking.
The time of the evening meal should also be altered so that there is adequate time for stomach emptying before lying down in bed. There should at least 4 hours between the last meal, snack or drink and bedtime. Therefore a person who normally retires to bed at 10 pm should not eat or drink after 6 pm.
Being overweight or obese contributes to acid reflux and therefore weight loss can have an effect on improving symptoms. Finally, an old fashioned remedy for persons who have acid regurgitation on lying down is to raise the head of the bed or to use many pillows to prevent having to lay completely flat. If these lifestyle changes have no significant effect on improving symptoms then the next step in treatment is with drugs.
The most common drug therapy associated with reflux symptoms is antacid liquids. These act by neutralizing the reflux acid but also help by encouraging the oesophagus to clear acid away. The most common antacid used is called Gaviscon.
The mainstay of treatment is drugs that will profoundly suppress the amount of acid that the stomach secretes. These drugs are called proton pump inhibitors (PPIs). The two most common of these drugs are Omeprazole (Losec) or Lansoprazole (Zoton). These drugs are highly effective in treating the symptoms of acid reflux disease. If a low dose of the drug does not work, the dose can be increased significantly from one tablet a day to up to three tablets twice a day. Most patients symptoms will be significantly improved with PPI therapy.
If the doctor considers that some of the acid reflux is caused by delayed gastric emptying, he may well prescribe a drug to help this. The most commonly prescribed of these drugs is Domperidone (Motilium). Some doctors may prescribe other medications such as H2 antagonist (Ranitidine, Cimetidine) or Bismuth compounds to help reflux disease. I do not personally think these are beneficial and therefore do not personally prescribe them.
Barrett’s oesophagus is a condition where frequent exposure of the lower oesophagus to acid leads to a change in the cellular lining of the oesophagus, from normal oesophagus cells to those resembling cells seen within the stomach. Barrett’s oesophagus is diagnosed by the observation that the darker red lining of the stomach appears to have migrated up into the lower oesophagus. The diagnosis is confirmed by biopsy of this area and analysing the cells under the microscope.
The concern with Barrett’s oesophagus is that changes to the cellular make up of the oesophagus increase the chance of the development of cancer. There are various grades of cellular changes called dysplasia. Type 1 signifies mild changes whereas Type 3 signifies severe cellular changes and can be associated with the very early stages of development of oesophageal cancer.
However, although there is a proven relationship between Barrett’s oesophagus and the development of cancer, it is in actual fact very rare occurrence. However unfortunately an element of hysteria has overshadowed the actual risks. A recent study from Denmark showed that in actual fact Barrett’s oesophagus developed into oesophagus cancer in only 1.2 per 1,000 patients per year. Even in those patients who had recognised precancerous cellular changes (dysplasia), only 5 per 1,000 patients per year developed oesophagus cancer (ref: Incidence of adenocarcinoma among patients with Barrett's esophagus. N Engl J Med. 2011 Oct 13;365(15):1375-83. Hvid-Jensen F et al).
A further study from Northern Ireland showed that patients who had Barrett’s oesophagus did not have any increased risk of dieing, compared to the general population (ref: Mortality in Barrett's oesophagus: results from a population based study. Gut. 2003 Aug;52(8):1081-4. Anderson LA et al).
Unfortunately drug therapy with acid suppression drugs (PPIs) has never been shown to stop Barrett’s oesophagus progressing into oesophagus cancer. There are several novel endoscopic therapies that attempt to destroy the Barrett’s segment, but there is conflicting data on the long term results of these therapies.
Anti-reflux surgery has so far been the only therapeutic intervention that has been shown to halt the progression of Barrett’s oesophagus. It has never however been shown to cause any regression of the condition.
However, as previously highlighted, although patients should be aware of what Barrett’s is and the potential risk of progression into cancer, they should always be reminded of the fact that this is an extremely unlikely occurrence, occurring in only 1-2 in 1,000 patients with Barrett’s per year.
Medical therapy has shown to be very effective in the treatment of reflux symptoms. Many patients are concerned about the risks of taking this medication in the long term for many years. There is no recognised long term risk from taking proton pump inhibitors.
Anti-reflux surgery is an extremely effective treatment for acid reflux disease. It is usually only indicated in a low proportion of patients who have not had a significant effect from acid suppression drug therapy, or do not want to take drug therapy long term.
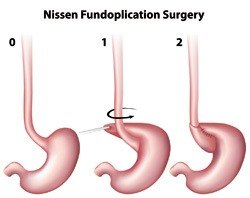
Anti-reflux surgery is performed via laparoscopic or keyhole surgery. It requires a general anaesthetic and the duration of the procedure is normally approximately one hour. A patient will stay in hospital usually for one night or occasionally two nights after surgery.
The operation involves the wrapping of the floppy upper part of the stomach (fundus) around the weakened lower oesophagus sphincter valve. This causes a much more effective and strong sphincter to prevent acid refluxing from the stomach into the oesophagus. In addition, the operation also involves the reduction and repair of any hiatus hernia that is present.
Anti-reflux surgery is as safe as most other types of routine surgery such as gallbladder removal or groin hernia repair. Any type of surgery however can involve some potential risks which in this procedure include bleeding, infection, damage to any of the organs in the region such as stomach or oesophagus and difficulty swallowing following the operation.
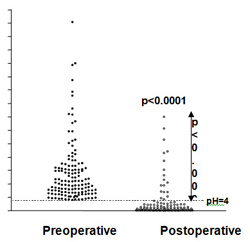
In patients who are refractory to drug treatment, anti-reflux surgery normally has an excellent effect in curing their symptoms. The vast majority of patients will no longer need to take any type of acid suppression drug and will not notice any further symptoms such as heartburn or acid regurgitation following surgery.
 There are, however, common side effects to the operation that a patient needs to be aware of. Because the new valve can sometimes be tight, this can lead to an initial difficulty with swallowing, particularly of dry foods such as bread and chicken. Some persons may have a significant problem with swallowing and require an endoscopic dilatation, or stretching of the valve, via a gastroscopy to fix this. In the vast majority of patients however, any initial difficulty swallowing will settle within days or weeks. Other common side effects include difficulty with belching or vomiting. This can cause an increased build up of gas within the stomach, the feeling of bloating in the abdomen and increased passage of flatus and/or diarrhoea. Again, these side effects will settle down within a few weeks of the operation.
There are, however, common side effects to the operation that a patient needs to be aware of. Because the new valve can sometimes be tight, this can lead to an initial difficulty with swallowing, particularly of dry foods such as bread and chicken. Some persons may have a significant problem with swallowing and require an endoscopic dilatation, or stretching of the valve, via a gastroscopy to fix this. In the vast majority of patients however, any initial difficulty swallowing will settle within days or weeks. Other common side effects include difficulty with belching or vomiting. This can cause an increased build up of gas within the stomach, the feeling of bloating in the abdomen and increased passage of flatus and/or diarrhoea. Again, these side effects will settle down within a few weeks of the operation.
The main message however is that if reflux is a real problem for you then surgery to fix this is safe and highly effective. Most people are extremely satisfied with the results of surgery.